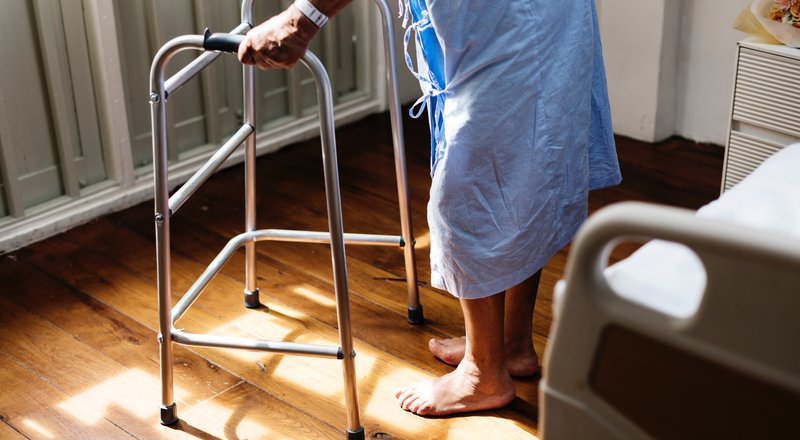
Medicare Advantage covers walkers, shower chairs, bed rails, raised toilet seats, bedside commodes, and wheelchairs after a hospital discharge under the DME (Durable Medical Equipment) benefit. Your doctor or discharge coordinator can order this equipment before you leave, and most plans deliver it within 24 to 48 hours at little or no cost to you.

Medline Aluminum Folding Rollator Walker
$80-130 · Covered under DME benefit ·
The answer is: quite a lot. And the key is asking before you leave.
The DME Benefit: Your Most Important Benefit After Discharge
Most of the equipment you need after a hospital stay falls under the DME (Durable Medical Equipment) benefit. This is a standard benefit in all Medicare Advantage plans. It covers equipment your doctor prescribes as medically necessary for use at home.
Your doctor or the hospital's discharge coordinator handles the prescription. Your plan handles the delivery. In most cases, there is no out-of-pocket cost to you beyond your normal copay.
What Equipment Is Covered?
Common DME items covered after hospital or rehab discharge fall into three main categories:
Mobility Equipment
Rollator walkers and standard walkers are the most commonly ordered DME items after discharge. Canes and quad canes (four-point base canes) provide lighter support for patients who are further along in recovery. Transport wheelchairs and standard wheelchairs are covered for patients with more limited mobility. Knee walker scooters are a common choice for foot and ankle surgery recovery because they allow hands-free mobility around the home.
Bathroom and Toileting Equipment
Shower chairs and bath benches make it possible to bathe safely while recovering. Raised toilet seats reduce the strain of sitting and standing, which is critical after hip or knee surgery. Bedside commodes are essential for patients who cannot safely walk to the bathroom during the early days of recovery. These items are inexpensive and dramatically reduce the risk of falls during the most vulnerable period after discharge.
Bedroom and Transfer Equipment
Hospital bed rentals are covered for patients who are mostly bed-bound and need an adjustable sleeping surface. Adjustable bed rails prevent falls during sleep and provide leverage for getting in and out of bed. Transfer boards and sliding boards help patients move safely between bed, wheelchair, and car. Power lift recliners are covered for patients who cannot safely rise from a standard chair.
The Most Important Rule: Ask Before You Leave
Once you are discharged, getting equipment arranged takes significantly longer and involves more back-and-forth between your doctor, your plan, and the DME supplier. When the discharge team is finalizing your paperwork, that is the moment to ask: "What equipment will I need at home? Can we get the order placed today?"
Most hospitals have a discharge coordinator or social worker whose job is to arrange exactly this. If no one has brought it up by the day before your discharge, ask to speak with the discharge coordinator directly.
What Your Doctor Needs to Do
For DME to be covered, your physician needs to write a prescription or order documenting medical necessity. This does not have to be a formal printed prescription. For most items, a verbal order documented in your chart is sufficient to start the process.
Ask your doctor or the hospital team before discharge: "Can you put in an order for a walker, shower chair, or commode so my plan can arrange delivery?"
How Fast Can Equipment Be Delivered?
For most standard items, delivery takes 24 to 48 hours after the order is placed. DME suppliers work closely with hospitals and plans to coordinate discharge equipment. In many cases, items like walkers and commodes can be delivered to your home before you arrive back from the hospital.
Hospital beds typically take 24 to 72 hours. More specialized equipment may take longer. Starting the process before discharge is the best way to avoid a gap.
Can You Use Both DME and Home Safety Benefits Together?
Yes. The DME benefit covers equipment. Grab bars, ramps, and home modifications fall under a separate benefit: the Home Safety benefit. Both can be used at the same time and both are commonly needed after a hospital or rehab stay. If you are setting up your home for a return from the hospital, you may qualify for both simultaneously.
What to Ask the Discharge Team Before You Leave
Before discharge, ask the coordinator, your nurse, or your doctor:
- "What equipment will I need at home to be safe?"
- "Can you place a DME order before I leave?"
- "Does my plan cover home safety modifications like grab bars? Who do I call?"
- "Will I have a home health nurse visiting after discharge?"
- "Can the home health team do a safety assessment when they visit?"
Writing these questions down before discharge day makes a real difference. Discharge day is busy and rushed. Having a list in hand ensures nothing gets missed.
What If You Already Came Home Without Ordering Equipment?
It is not too late. Call your plan's Member Services line and explain that you recently returned from a hospital or rehab stay and need DME. Ask them to connect you with an in-network DME supplier. You will need your doctor to submit an order, which your plan or the DME supplier can help coordinate.
The process takes a few extra days compared to arranging it before discharge, but the coverage is the same.
Official Medicare Resources