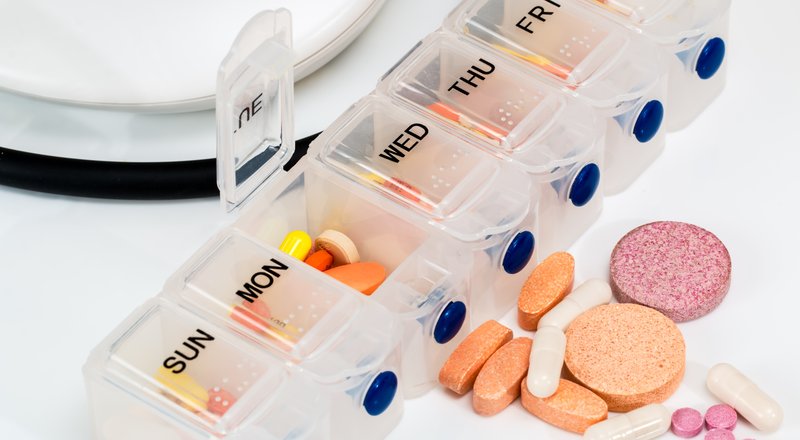
Most Medicare Advantage members receive an OTC (Over-the-Counter) benefit, a quarterly or annual allowance to spend on health and wellness products. The average allowance is $100 to $200 per quarter, though some plans offer significantly more. Most members use less than half of what they are entitled to, simply because they do not know what the benefit covers.
Omron Wireless Wrist Blood Pressure Monitor
$40-80 · Covered under OTC benefit ·
Here is a comprehensive breakdown of what the OTC benefit covers and how to use it.
What Is the Medicare Advantage OTC Benefit?
The OTC benefit is a supplemental benefit that gives you a pre-loaded allowance to spend on approved health items. Original Medicare does not offer this benefit, it is one of the key advantages of Medicare Advantage plans over Original Medicare.
Depending on your plan, you can use your OTC allowance by:
- Ordering items from your plan's online catalog (most common)
- Ordering by phone through your plan's OTC vendor
- Shopping in-store at approved retailers (CVS, Walgreens, Walmart, Rite Aid, and others depending on your plan)
The allowance resets quarterly or annually depending on your plan. Unused funds typically do not roll over.
What Can You Buy With the OTC Benefit?
OTC catalogs vary by plan, but most include items across these categories:
Monitoring and diagnostics:
- Blood pressure monitors (upper arm and wrist)
- Pulse oximeters
- Blood glucose meters and test strips
- Thermometers
- Weight scales
Pain relief and physical therapy:
- TENS units for muscle and joint pain
- Heating pads and ice packs
- Over-the-counter pain relievers (acetaminophen, ibuprofen, naproxen)
- Topical pain creams and patches
- Back supports and braces
- Knee and ankle supports
Vitamins and supplements:
- Multivitamins
- Vitamin D and calcium supplements
- Fish oil and omega-3 capsules
- Magnesium, zinc, and B vitamins
- Fiber supplements
Incontinence and skin care:
- Adult incontinence pads and briefs
- Waterproof mattress protectors
- Skin barrier creams and wound care supplies
- Moisturizing lotions and ointments
Dental, vision, and hearing:
- Toothbrushes, toothpaste, and dental floss
- Denture adhesives and cleaners
- Reading glasses (non-prescription)
- Hearing aid batteries
Fall prevention and safety:
- Non-slip bath mats
- Motion-sensor night lights
- Bed exit alarms
- Compression socks and stockings
- Gait belts and transfer aids
- Reachers and grabbers
- Dressing aids (sock assist, long-handled shoehorn)
First aid and wound care:
- Bandages, gauze, and medical tape
- Antiseptic solutions
- First aid kits
What Does the OTC Benefit NOT Cover?
OTC benefits do not typically cover:
- Prescription medications
- Food, beverages, or meal supplements (unless your plan has a separate Healthy Food benefit)
- Personal care products like shampoo or soap (unless specifically listed in your catalog)
- Medical equipment that falls under the DME (Durable Medical Equipment) benefit (walkers, wheelchairs, hospital beds)
- Any item not listed in your plan's approved catalog
How Much Is the OTC Allowance?
The amount varies significantly by plan and year. Common ranges:
- Basic plans: $25 to $50 per quarter ($100 to $200 per year)
- Mid-tier plans: $75 to $150 per quarter ($300 to $600 per year)
- Premium plans: $200+ per quarter ($800+ per year)
OTC Allowance by Major Carrier (2026 Plans)
| Carrier | Typical Quarterly Allowance | Annual Total | How to Order |
|---|---|---|---|
| UnitedHealthcare | $30 - $200+ | $120 - $800+ | Online, phone, or Walmart/Walgreens in-store |
| Humana | $25 - $150+ | $100 - $600+ | Online catalog, phone, or CVS/Walgreens in-store |
| Aetna | $25 - $125+ | $100 - $500+ | Online catalog or phone order |
| Anthem BCBS | $35 - $175+ | $140 - $700+ | Online, phone, or Walmart in-store |
Note: Amounts vary by specific plan within each carrier. Check your Summary of Benefits for your exact allowance.
Your specific allowance is listed in your plan's Annual Notice of Change or Summary of Benefits. If you do not know your allowance amount, call Member Services or log in to your plan's member portal.
How to Check Your OTC Balance
The easiest ways to check your remaining balance are:
- Log in to your plan's member portal or app
- Call the OTC benefit line on the back of your insurance card
- Check at checkout when shopping in-store at an approved retailer
Do OTC Funds Roll Over?
In most plans, unused OTC funds do not roll over to the next period. If your allowance resets quarterly, any balance remaining at the end of the quarter is forfeited. This is the primary reason members leave money unused, they do not realize the deadline until it is too late.
Set a reminder two weeks before the end of each quarter to check your balance and place an order if you have remaining funds.
Can You Use the OTC Benefit at CVS, Walgreens, or Walmart?
Many plans allow in-store purchases at major pharmacy retailers. However, the specific retailers and which items are eligible vary by plan. You typically need to select eligible items (marked in the store's system) and present your insurance card or a specific OTC card at checkout. Ask Member Services for a list of approved in-store retailers and how to identify eligible items.
Official Medicare Resources